|
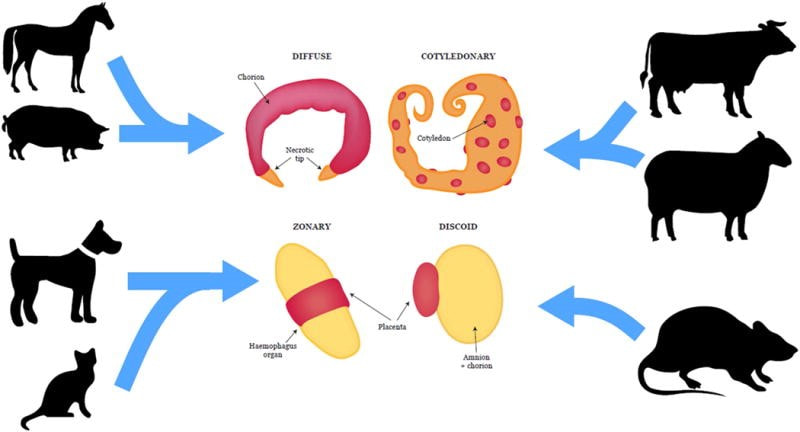
Being able to shelter a baby inside the womb for 9 months is something I have always found fascinating. Not only is it a beautiful result of natural adaptation, but pregnancy is also a risky situation during which an efficient compromise needs to be reached between the baby, who needs the mother’s resources, and the mother who needs to cope with the huge challenge of transforming her own body for the benefit of her baby. Maintaining this equilibrium would be impossible without the placenta, which performs an impressive number of tasks to keep both the baby and the mother safe from fecundation to birth. And yet, the placenta has never really received the attention it deserves. Not only by the general public, which often only has vague ideas about what a placenta does, but even more sadly, by the scientific community. The placenta is the least studied organ of the human body and still holds many mysteries. I wasn’t too sure myself about what a placenta did exactly before starting my PhD. I have to say that since then, I have never stopped being amazed at its multi-faceted capacities. With this article, I would like to put the placenta under the spotlight for a moment by sharing with you some of what I found are its most astonishing powers. 1. The placenta helped the transition from marine to terrestrial life The formation of a placenta was a turning point in the evolution of breeding strategies by helping the transition from laying eggs (oviparity) to giving birth to live babies (viviparity). The first amphibians and reptiles emerging from the sea over 300 million years ago bred by laying eggs, and many still do. After the egg is laid, the embryo gets its food from the yolk to grow until the time of hatching. In a few reptiles, instead of being laid, the egg started to hatch inside the mother’s womb and remained attached for long periods. In this arrangement, the eggshell was modified into a specialized organ, called the placenta, allowing the embryo to directly access nutrients from the mother’s blood. This strategy provided an evolutionary advantage by allowing the embryo to feed, breathe and grow safely inside the womb throughout the gestation period. Protected from predators, these live-bearing reptiles were the most successful to colonize the lands during the Mesozoic era, which became the “Age of reptiles”. 2. The placenta is the most variable organ in the animal kingdom Apart from a few exceptions, most mammals have developed a placenta. Contrary to other organs, which exhibit roughly similar forms and functions across mammal species, placentas come in an almost infinite variety of shapes, sizes and structures (see figure below). They also invade the uterus at different degrees. The human placenta is unique in that regard as it penetrates the most deeply within the uterus wall, destroying blood vessels and coming in direct contact with the mother’s blood. At the opposite extreme, the placenta of species like sheep merely attaches superficially to the surface of the uterus. Some are in between. The horse placenta, for example, is essentially non-invasive but grows local structures penetrating the uterus, called “placental cups”. Figure: Placental morphologies of varying placental mammals. Taken from Roberts et al, 2016 [1] As you may notice from the examples, similar placenta types were adopted by unrelated species and conversely, a diversity of placental structures can be seen within species of a same group. This tells us that this organ did not follow the established evolutionary relationships. Rather than evolving from a single primitive form, placentas actually evolved multiple times throughout the animal kingdom, and independently. As a result, some forms of placentas can now be found in a wide diversity of animals, even some very far from mammals. The poecilid fish mothers, instead of laying eggs as most fish do, keep their offspring inside their bodies and developed an organ to pass nutrients over to the growing baby. Even further from mammals, many flowering plants developed a tissue specialised in the transfer of resources from the mother plant to the embryonic seed. Despite being anatomically far from mammal placentas, those structures do the same job. This “convergent evolution” shows how useful a placenta-like function can be regardless of the species, and the diversity of strategies adopted by living beings to build one is a great illustration of nature’s inventiveness. Why so many types? In which order did they evolve? We are still far from knowing the whole story, which remains a source of fascination and an enigma for evolutionary biologists. 3. Some placenta properties were acquired from a virus infection more than 25 million years ago Although many viruses cause serious diseases like AIDS, measles, or the sadly famous covid-19, they can also prove to be very useful for humans. As they infect individuals, viruses insert their own genes into the host DNA. When inserted within a sperm or egg cell, this new piece of genetic information can be retained and transmitted to the next generations via what is called “vertical transmission”. That is how many viral genes have been permanently integrated in the human genome. In fact, scientists estimated that about 8% of our genome is made up of viral genes! [2] Some of those genes continue to produce viral proteins, sometimes for our own benefit. The syncytin protein is one of them. Originally present on viruses’ surface, syncytin allows the virus entry into its target cell by fusing their membranes together.. Some primates, which received this precious gene within their own DNA after an ancient viral infection, took great advantage of its fusion activity. As it does for viruses, the syncytin now also fuses placental cells together to form a highly specialised external shell in direct contact with the mother’s blood. Although the idea of using a viral protein can be surprising, it could prove to be a very good thing. As syncytin uses viral pathways to fuse cells, it competes with other potential harmful viruses that would need to use the same pathways to infect the placenta and the baby. In other words, a virus helped us fight… viruses. But the placenta probably gained much more from viruses than only syncytin. A growing number of viral proteins are emerging as important players in the evolution of our placental form of reproduction, likely helped by multiple infections throughout the years [3]. 4. The placenta takes the role of human lungs, digestive tract, kidneys and immune system at the same time It is not until after birth that the baby’s vital systems are fully functioning. In the meantime, the growing foetus relies on the placenta to play the role of various organs for it. This is made possible by the reciprocal exchange of products between the mother’s and the baby’s blood, taking place at the placental interface. Gases, for example, can easily transit from one to another. Therefore, the foetus takes oxygen from the mother and disposes of its carbon dioxide in the other direction. In other words, what the future lungs will do. As for the feeding, essential energetic compounds in the food consumed by the mother are transported to the baby to boost its growth, and metabolic wastes are eliminated in the other direction. However, not everything can cross the placenta. Its high selectivity allows it to prevent any harmful compound from reaching the baby, such as toxic substances or pathogens. This filtering activity resembles the job of the skin after birth. In addition, an initial set of maternal antibodies is transferred as an initial protection of newborns against most bacterial infections. As soon as the baby is born, its own lungs, digestive system, kidneys and immune system will take over. 5. The placenta has long term impacts on the baby and the mother We already talked about the multiple roles of the placenta in assisting the baby’s growth during pregnancy. But something less known is how crucial a good placental function is for the mother’s and the baby’s health later in life. The placenta, indeed, has the tremendous responsibility of assisting the development of some of the baby’s core health parameters that will last for life. Of course, everyone’s traits are initially determined by our genes. But the uterine environment in which we grow during our first 9 months plays a substantial role in shaping our future. The food intake is a good example for that. If a baby is undernourished in the womb, its metabolism and energy consumption will adjust to food deprivation to store more fat provisions. Although the food availability may increase after birth, this metabolism is already in place and will remain. Hence, undernourished embryos are exposed to increased risks of obesity, diabetes and other cardiovascular diseases later in life [4]. Some astonishing examples of the effects of food on embryos’ development can be found in insects. What determines if a bee will become a queen or a worker has nothing to do with genetics: all comes down to the food intake of the larva. If a larva is fed with royal jelly instead of the regular meal, the development of its body and brain will be diverted so that the future bee will look like and behave like the queen of the colony. The placenta does not only programme the baby’s life. The massive amounts of hormones it releases throughout pregnancy are powerful modulators of the mother’s body. During pregnancy, they act as a continuous signal to make the mother’s body aware of the pregnancy and sustain it throughout the 9 months. But the effects of placental hormones do not end at birth. In fact, they may well help a lot in the first months of life. Not only some of them stimulate milk production in order to prepare for future breast feeding, but some may even influence the mother’s behaviour to foster nurturing and bonding with the young. Given that the placenta is made of the fetus’s cells, are mothers actually manipulated by the baby to ensure they bring the care it needs? This may sound like rather a negative perspective, but one thing is certain: the effects of placental hormones on the brain are being studied with great interest within the scientific community and show the wide extent of maternal body functions impacted by placental functions. This is a great power when it is functioning properly. But the downside is that placental malfunctions can lead to long-term adverse outcomes for the mother. Women who suffered from preeclampsia, during which the placenta fails to develop normally, are at higher risk of developing cardiovascular diseases later in life. These examples show that a good placental function is of crucial importance, and even minor alterations can result in serious life-long consequences. 6. Studying the placenta could help us cure cancer As scary as it might sound, pregnancy and tumours have a lot in common. Here is a non-exhaustive list of shared features, showing that understanding common and divergent pathways between placentas and tumours could have various practical utilities in improving healthcare. A. Both escape the immune system of the host. Because the placenta is made of the baby’s cells, it should be detected as a foreign intruder by the mother’s body and be targeted by her immune system. And yet, it peacefully makes its way through the uterus during 9 months without being rejected. This paradox has been fascinating immunologists for a very long time, and we are still far from understanding exactly how this state of peace is reached and maintained. At least some strategies are shared between placentas and tumours for escaping the host immune system. Both lack the usual identity markers normally expressed on the cell surface, which signal to the immune system whether the cell belongs to the same organism and should be trusted or is an intruder that would better be eliminated. Instead, placental cells display very unusual signals allowing them to hide from the immune system. Understanding those mechanisms better could give us insights about tumour tolerance. It could also inspire new strategies to avoid rejects of organ transplants. B. Both release similar products. Some proteins, normally produced during pregnancy only, are reactivated within certain kinds of cancers. Those are called “oncofetal” proteins, reflecting their dual functions in foetal development and cancer growth. Their function is generally to stimulate cell growth and bypass programmed death, sustaining the placenta or ensuring survival of the tumour. The well-known human chorionic gonadotrophin (hCG), quantified in pregnancy tests, is one of them. C. Both are highly invasive. Like tumours, the placenta deeply invades the host organism and draws on its resources to grow. The strategies employed by placental cells to migrate and invade the maternal uterus have been extensively compared with tumour cell invasion of other organs: both make their ways through the “foreign” organs by degrading tissues and eventually destroy its blood vessels. Apart from the uterus, the placenta can theoretically implant and invade almost every organ in the body, provided that enough blood is accessible to sustain its growth. In rare cases, the placenta implants outside of the uterus; most often in fallopian tubes, but sometimes even in the intestine. The presence of an invading placenta in those abnormal locations is a high-risk situation requiring urgent intervention. As incredible as it may seem, healthy babies were born from such pregnancies [5]. Despite this similar invading potential, some key differences exist between both entities and those distinctions are what interest the researchers most. Unlike tumours, which grow and invade uncontrollably and even reach new tissues, the placental invasion is a highly controlled process. It sticks to a tightly regulated pattern under the regulation of maternal factors, preventing it from invading too far in the uterus. Are placental cells mimicking cancerous cell behaviour, or are cancer cells mature cells coming back to an embryonic behaviour? What makes the placental invasion so tightly controlled? Answering those questions could give us precious insights into how we could control tumour growth, and reciprocally, some tumour strategies could prove useful to resolve placental deficiencies. References: Articles [1] Roberts, R. M., Green, J. A., & Schulz, L. C. (2016). The Evolution of the Placenta. Reproduction, 152(5), R179–R189. https://doi.org/10.1530/REP-16-0325.The [2] McPherson, J.D., Marra, M., Hillier, L., Waterston, R. H., Chinwalla, A., Wallis, J., Sekhon, M., Wylie, K., Mardis, E. R., Wilson, R. K. et al. (2001). A physical map of the human genome. Nature 409, 934-941. doi:10.1038/35057157 [3] Chuong, E.B. (2018). The placenta goes viral: Retroviruses control gene expression in pregnancy. PLoS Biol 16(10): e3000028. https://doi.org/10.1371/journal.pbio.3000028 [4] Fall, C. (2013). Fetal malnutrition and long-term outcomes. Nestle Nutrition Institute Worksop 74, 11-25. Doi:10.1159/000348384 [5] Baffoe, P., Fofie, C., & Gandau, B. (2011). Term abdominal pregnancy with healthy newborn : a case report. Ghana medical journal 46(2), 81-83 Books Y. W. Loke, Life’s Vital Link: The Astonishing Role of the Placenta. Oxford University Press, USA, 2013. AuthorAgathe Lermant is an Early Stage Researcher of iPlacenta. Read her earlier blog post here.
Leave a Reply. |
About the blogBeing a PhD student in a European training network is a life-changing adventure. Moving to a new country, carrying out a research project, facing scientific (and cultural) challenges, travelling around Europe and beyond… Those 3 years certainly do bring their part of new - sometimes frightening - but always enriching experiences. Categories
All
Archives
December 2021
|





 RSS Feed
RSS Feed

18/6/2020
1 Comment